 Goal: maximize the ability to communicate. Objective data: the words are difficult to understand, face rigid.Subjective Data: client / family says the difficulty in talking.Nursing Diagnosis Impaired Verbal Communication related to the decline in speech and facial muscle stiffness teach and support the client during the client's activitiesģ.collaborative provision of laxatives and consult a doctor of occupational therapy.avoid what not to do the client and help if needed.assess the ability and the rate of decline and the scale of 0-4 to perform ADL.Nursing Diagnosis Self care deficit related to neuromuscular weakness, decline in strength, loss of muscle control / coordination.Įxpected results: the client can indicate a change of life for the needs of taking care of themselves, clients are able to do self-care activities in accordance with the level of ability, and identify personal / community that can help. collaboration physiotherapists for physical exerciseĢ.help clients perform ROM exercises, self-care according to tolerance.encourage hangan bath and massage the muscle.do an exercise program increases muscle strength.examine existing mobility and observation of an increase in damage.Nursing Interventions for Parkinson's Disease : Goal: The client is able to perform physical activity according to ability.Įxpected results: the client can participate in training programs, joint contractures did not occur, increased muscle strength and the client indicates an act to increase the mobility Nursing Diagnosis Impaired physical mobility related to the stiffness and muscle weakness. Jun Yu, Movement Disorders Fellow at the University of Florida, a Parkinson’s Foundation Center of Excellence.1. For this reason, researchers focus on these non-motor symptoms to detect PD as early as possible and to look for ways to stop its progression. This theory is supported by evidence that non-movement symptoms, such as a loss of sense of smell, sleep disorders and constipation, may appear several years ahead of movement symptoms. The aggregated α-Synuclein (called Lewy body) then spreads toward the central nervous system (namely the brain), and eventually arriving in and causing the degeneration of the dopaminergic neurons in the area of the brain called the substantia nigra. The pathogenic products thus come into contact with the olfactory (smell) and/or enteric (gut) neurons, triggering the aggregation of an abnormal protein called α-Synuclein. In this theory, the pathogen enters the body via the nose and/or gets swallowed and reaches the gut. This was followed by a more extensive hypothesis, stating that PD starts in two places: the neurons of the nasal cavity and the neurons in the gut. In 2003, Heiko Braak, MD, hypothesized that an unknown pathogen (a bacteria, virus or other microorganism that causes disease) in the gut could be the cause of PD. Researchers believe a combination of genetic and environmental factors cause Parkinson’s. Theory of PD Progression: Braak’s Hypothesis Increasingly, clinicians and researchers are exploring new kinematic sensor technologies to help detect and measure motor symptoms and fluctuations. They may provide invaluable insights on motor fluctuations in relation to medication intake. On this scale, stages 1 and 2 represent early-stage, 2 and 3 mid-stage, and 4 and 5 advanced-stage PD. Clinicians use it to describe how motor symptoms progress in PD. In 1967, Hoehn & Yahr defined five stages of PD based on the level of clinical disability. Postural instability (trouble with balance and falls) typically occurs after about 10 years. Motor fluctuations can become an issue five to 10 years after diagnosis. 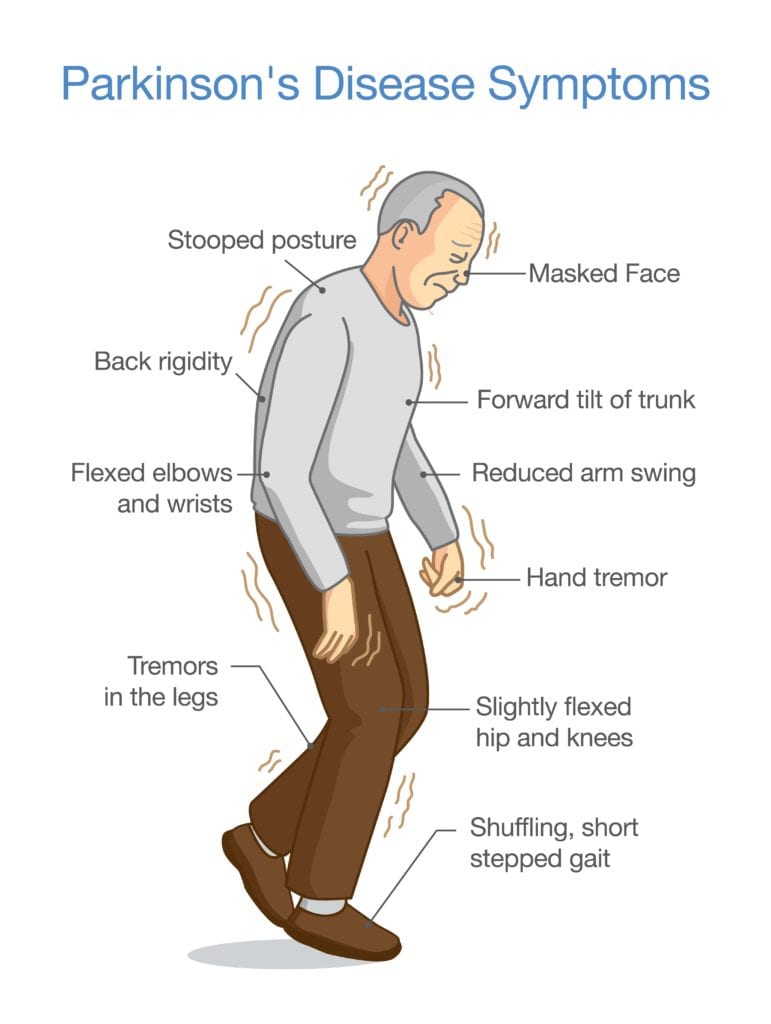
People with young-onset PD are more prone to levodopa-induced dyskinesia and changes in movement (called motor fluctuations), while those diagnosed later in age may experience more cognitive changes and non-movement symptoms. In this timeframe, they may experience new or worsening movement symptoms and fluctuations, levodopa-induced dyskinesia, swallowing problems, freezing of gait, falls and imbalance. However, as the disease progresses, people with Parkinson’s often need to work alongside their doctor to adjust levodopa dosages. 
This optimal timeframe can last many years and varies for everyone. Following a diagnosis, many people experience a good response to medications, such as levodopa. It is difficult to accurately predict the progression of Parkinson’s. Others find the disease progresses more quickly. Some people experience the changes over 20 years or more. While symptoms and disease progression are unique to each person, knowing the typical stages of Parkinson’s can help you cope with changes as they occur. 
Not everyone will experience all the symptoms of PD even if people do, they won’t necessarily experience the symptoms in quite the same order or at the same intensity. Parkinson’s disease (PD) impacts people in different ways. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
